Introduction
We live in a culture that glorifies busyness. Hustle culture tells young people to grind through sleepless nights, juggle multiple commitments, and push through stress like it is a badge of honor. “I’ll sleep when I’m dead” has become a mantra for ambitious millennials and Gen Z. But here is the cruel irony: by neglecting sleep and ignoring chronic stress, you are accelerating exactly what you are trying to outrun—an early death.
The medical community is now sounding the alarm on a silent epidemic that isn’t about cholesterol or obesity, but about the invisible wear and tear of modern life on young hearts. Chronic stress and sleep deprivation are not just uncomfortable; they are independent, direct risk factors for heart attacks, strokes, and sudden cardiac death—even in people who look perfectly healthy on the outside.
In our previous articles, we explored the broader crisis of heart attacks in youth and the specific dangers of energy drinks and pre-workout supplements. Now, we turn to the hidden drivers that often go unnoticed: the relentless pressure of daily life and the cumulative debt of missed sleep. Chronic stress and sleep deprivation are the silent assassins of the modern era.
This article uncovers the six devastating ways chronic stress and sleep deprivation damage your cardiovascular system, shares real-life stories of young people who paid the ultimate price, and provides actionable strategies to reverse the damage before it is too late.
What Are Chronic Stress and Sleep Deprivation?
To understand how chronic stress and sleep deprivation destroy the heart, we need to define them clearly. They are not just feelings of being “stressed out” or “tired.” They are physiological states with measurable biological consequences.
Chronic Stress
Unlike acute stress—the brief adrenaline rush before a presentation or competition—chronic stress is the prolonged, unrelenting activation of the body’s stress response. It can stem from:
- Financial pressure and student debt
- Demanding jobs with unrealistic expectations and long hours
- Toxic relationships or caregiving responsibilities
- Social media anxiety and constant comparison
- Academic pressure and performance expectations
- Uncertainty about the future and career instability
When stress becomes chronic, the body’s hypothalamic-pituitary-adrenal (HPA) axis stays switched on, flooding the system with cortisol and adrenaline for weeks, months, or even years. This constant activation means chronic stress and sleep deprivation often go hand in hand, creating a vicious cycle.
Sleep Deprivation
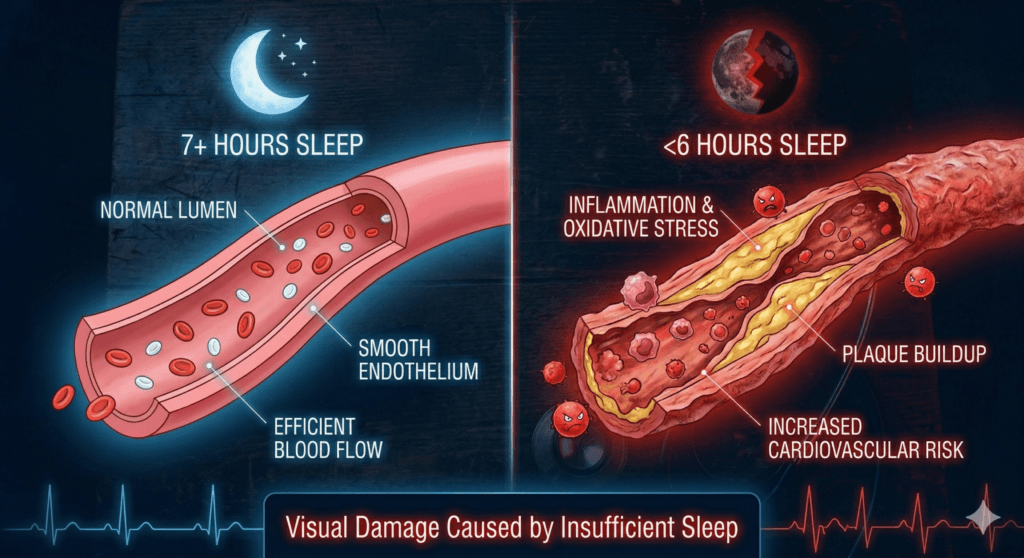
Sleep deprivation isn’t just about feeling tired. It is defined as regularly getting less than 7 hours of quality sleep per night. For young adults, this has become alarmingly common—over one in three adults under 40 report sleeping less than 7 hours on weeknights. Chronic sleep deprivation impairs every organ system, with the cardiovascular system being among the hardest hit.
Together, chronic stress and sleep deprivation create a perfect storm that accelerates atherosclerosis, destabilizes heart rhythms, and dramatically increases the risk of sudden cardiac events. They are not separate problems; they feed into each other in a destructive feedback loop.
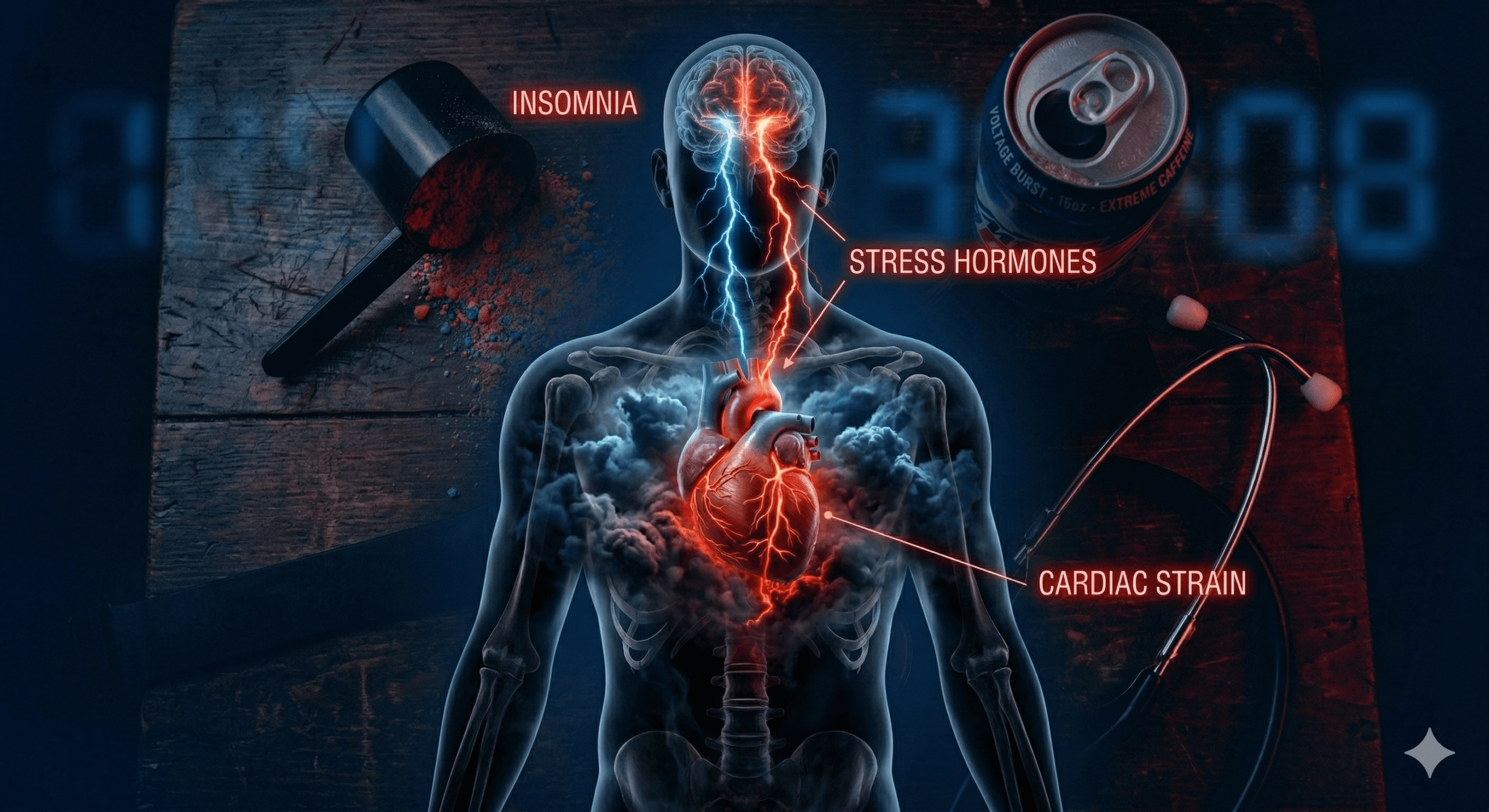
How They Work: The Biological Assault on Your Heart
Let’s walk through what happens inside a young body under constant chronic stress and sleep deprivation. The biological assault unfolds through multiple interconnected mechanisms.
The Cortisol Cascade
When you are chronically stressed, your adrenal glands pump out cortisol. In small doses, cortisol is helpful for alertness and energy. But chronically elevated cortisol:
- Increases blood pressure by constricting blood vessels and increasing fluid retention
- Raises blood sugar, promoting inflammation and arterial damage over time
- Increases visceral fat—the dangerous fat stored around internal organs that actively contributes to heart disease
- Promotes plaque formation by encouraging LDL cholesterol to embed in artery walls
- Suppresses immune function, making the body less able to repair vascular damage
This cortisol cascade is a primary mechanism by which chronic stress and sleep deprivation damage the cardiovascular system.
The Autonomic Imbalance
Your autonomic nervous system has two branches: sympathetic (fight or flight) and parasympathetic (rest and digest). Chronic stress and sleep deprivation tip the balance heavily toward sympathetic dominance. This means:
- Your resting heart rate stays elevated, even when you are trying to relax
- Your heart rate variability (HRV) drops—a key marker of cardiovascular resilience that predicts heart attack risk
- Your heart becomes more susceptible to arrhythmias and electrical instability
- Your blood vessels remain constricted, raising blood pressure around the clock
This autonomic imbalance means your heart never gets the break it needs. Chronic stress and sleep deprivation keep your cardiovascular system in a perpetual state of high alert.
The Inflammatory Response
Sleep is when the body clears inflammatory markers. During deep sleep, the brain activates the glymphatic system to remove waste products, and the cardiovascular system undergoes repair. When you don’t sleep, C-reactive protein (CRP) and interleukin-6 (IL-6) —both powerful inflammatory molecules—remain elevated.
Inflammation is the spark that ignites plaque rupture. A person suffering from chronic stress and sleep deprivation walks around with chronic low-grade inflammation that primes their arteries for disaster. This inflammatory state is a key reason why chronic stress and sleep deprivation are now recognized as independent risk factors for heart attacks.
The Endothelial Dysfunction
The endothelium is the inner lining of your blood vessels. It is responsible for regulating blood flow, preventing clots, and repairing damage. Chronic stress and sleep deprivation directly damage the endothelium, causing it to become stiff and dysfunctional. When the endothelium fails, plaque can form more easily, and clots become more likely. This endothelial damage is a silent process that occurs years before any symptoms appear.
Real-World Cases: When Stress and Sleeplessness Turn Deadly
These aren’t theoretical risks. These are real lives where chronic stress and sleep deprivation led to devastating cardiac events.
Case Study 1: The Medical Resident
Profile: Female, 29 years old. Medical resident working 80-hour weeks. Fit, non-smoker, no family history of heart disease. She was in the prime of her career and physical health.
The Event: After a 28-hour shift—common in medical training—she collapsed in the hospital cafeteria from sudden cardiac arrest. Fortunately, colleagues performed CPR immediately, and she was revived.
The Cause: Extreme sleep deprivation combined with the relentless stress of residency caused her heart muscle to “stun” itself. She was diagnosed with Takotsubo cardiomyopathy—stress-induced heart failure often called “broken heart syndrome.” Her coronary arteries were clean, but the stress hormones from chronic stress and sleep deprivation literally weakened her heart to the point of failure.
Case Study 2: The Startup Founder
Profile: Male, 32 years old. Founder of a high-growth tech startup. Worked 7 days a week, slept 4–5 hours nightly, consumed caffeine constantly to stay alert. He was living the “hustle culture” dream.
The Event: During a pitch meeting with potential investors, he experienced sudden chest tightness, jaw pain, and collapsed. He was rushed to the hospital and diagnosed with a massive anterior wall myocardial infarction—the “widowmaker” heart attack.
The Cause: Years of chronic stress and sleep deprivation accelerated his underlying plaque buildup. At 32, he had the arteries of a 60-year-old. He survived but required emergency bypass surgery. His cardiologist stated that without the chronic stress and sleep debt, his heart attack likely would not have occurred for decades.
Case Study 3: The Single Mother
Profile: Female, 26 years old. Single mother of two young children, working two jobs to make ends meet. Constant financial stress, sleeping in 2–3 hour increments for months. She was doing everything she could to provide for her family.
The Event: She began experiencing episodic palpitations and shortness of breath. One night, she woke up with severe chest pain radiating to her back and was rushed to the ER. She was diagnosed with spontaneous coronary artery dissection (SCAD) —a tear in the wall of her coronary artery.
The Cause: Extreme chronic stress and sleep deprivation are known triggers for SCAD, particularly in young women. Her cardiologist explained that the relentless physical and emotional toll on her body had weakened her arterial walls, making them vulnerable to tearing.
Case Study 4: The College Student
Profile: Male, 21 years old: college senior juggling finals, a part-time job, and intense social pressures. Regularly slept 4–5 hours, consumed energy drinks, and was constantly anxious about his future.
The Event: During final exams, he experienced sudden, crushing chest pain and collapsed in the library. Fellow students called 911. He was diagnosed with myocardial infarction with non-obstructive coronary arteries (MINOCA) —a heart attack without significant plaque buildup.
The Cause: Severe chronic stress and sleep deprivation triggered coronary artery spasm, cutting off blood flow to his heart. His cardiologist noted that his case is becoming increasingly common among young adults living under constant pressure.
Warning Signs: When Your Body Is Saying “Enough”
If you are suffering from chronic stress and sleep deprivation, your body may send these warning signals. Do not ignore them.
- Persistent fatigue that sleep doesn’t fix—you wake up tired even after 8 hours
- Frequent palpitations or sensation of skipped beats
- Chest tightness or pressure, especially during periods of high stress
- Shortness of breath with minimal exertion that wasn’t there before
- Dizziness or lightheadedness when standing up
- Difficulty recovering from exercise (heart rate stays elevated for hours)
- Brain fog and difficulty concentrating
- Increased anxiety or irritability without a clear trigger
- High blood pressure readings, even if you are young and fit
These symptoms are not “just stress.” They are physiological responses to chronic stress and sleep deprivation that warrant medical evaluation.

Future Impact: The Cardiovascular Debt
The concept of “cardiovascular debt” is gaining traction among cardiologists. Just as financial debt compounds interest over time, the damage from chronic stress and sleep deprivation accumulates and grows. The longer you live under these conditions, the greater the toll on your heart.
Early Onset Heart Failure
Young adults who survive heart attacks often face heart failure later in life. The scar tissue from a heart attack reduces the heart’s pumping ability. A 30-year-old heart attack survivor may have the cardiac function of a 60-year-old, facing decades of medication, lifestyle restrictions, and reduced quality of life. Chronic stress and sleep deprivation are major contributors to this early decline.
The Generational Toll
We are raising a generation that views chronic stress and sleep deprivation as normal. Unless we shift cultural norms, we will see a surge in cardiovascular disability among people in their 30s and 40s. This will place an enormous burden on healthcare systems, families, and the economy. The long-term costs of chronic stress and sleep deprivation are staggering.
The Role of Wearables and Early Intervention
The future will likely involve wearable devices that monitor not just steps, but heart rate variability, sleep quality, and stress indicators. These tools can provide early warnings, but only if individuals act on them—by prioritizing rest and stress management before a crisis occurs. Early detection of chronic stress and sleep deprivation can prevent devastating outcomes.
Workplace and Societal Changes
There is growing recognition that workplaces must address chronic stress and sleep deprivation as occupational health hazards. Forward-thinking companies are implementing:
- Mandatory time-off policies to prevent burnout
- Flexible schedules to allow adequate sleep
- Mental health resources and stress management programs
- Limits on after-hours communication
These changes are not just good for employees; they are essential for preventing the cardiac consequences of chronic stress and sleep deprivation.
Expert Opinion: Insights from Cardiologists and Sleep Specialists
To understand the true impact of chronic stress and sleep deprivation on young hearts, we consulted leading experts.
Dr. Matthew Walker, PhD, Professor of Neuroscience and Psychology, UC Berkeley, Author of Why We Sleep:
“Short sleep—less than seven hours a night—is one of the strongest predictors of heart attack and stroke. When you sleep, your heart rate drops, blood pressure lowers, and your blood vessels repair themselves. Without that nightly restoration, your cardiovascular system is in a constant state of stress. The link between chronic stress and sleep deprivation and heart disease is undeniable.”
Dr. Nieca Goldberg, MD, Medical Director of the Joan H. Tisch Center for Women’s Health at NYU Langone:
“I see young women all the time who are juggling careers, families, and social pressure. They come in with chest pain, palpitations, and sky-high blood pressure. Often their heart tests are normal initially, but the chronic stress and sleep deprivation are setting them up for disease down the road. We need to treat stress as a cardiac risk factor, just like high cholesterol.”
Dr. Michael Twery, PhD, Director of the National Center on Sleep Disorders Research:
“Sleep is not a luxury. It is a biological necessity. The evidence linking chronic stress and sleep deprivation to cardiovascular disease is as strong as the evidence linking smoking to lung cancer. We need to treat sleep as a vital sign.”
Dr. Aditi Nerurkar, MD, Harvard Medical School, Stress Expert:
“The problem with chronic stress and sleep deprivation is that they become normalized. Young people think it’s normal to be exhausted. It is not. When you chronically suppress your body’s need for rest, you are setting the stage for a cardiac event. We need to redefine what ‘normal’ looks like.”
Expert Takeaways:
- Treat sleep as non-negotiable: Aim for 7–9 hours consistently. It is as important as diet and exercise for preventing the effects of chronic stress and sleep deprivation.
- Build stress resilience: Incorporate mindfulness, therapy, or exercise not as luxuries but as medical necessities.
- Monitor your numbers: Check blood pressure regularly. Chronic stress and sleep deprivation often manifest as sustained hypertension.
- Create sleep hygiene: Consistent bedtime, dark room, no screens before bed—these are not optional for anyone dealing with chronic stress and sleep deprivation.
Recent Studies: The Science of Stress and Sleep
The medical literature increasingly confirms the devastating impact of chronic stress and sleep deprivation on cardiovascular health.
Study 1: Sleep Duration and Atherosclerosis
Published in Journal of the American College of Cardiology (2023)
Researchers studied nearly 4,000 adults aged 40–54, measuring coronary artery calcium (CAC) scores to detect early plaque buildup.
- Key Finding: Those who slept less than 6 hours per night had a 27% higher likelihood of having subclinical atherosclerosis (plaque buildup) compared to those sleeping 7–8 hours. This effect was independent of diet, exercise, and other risk factors, demonstrating that chronic stress and sleep deprivation directly contribute to arterial disease.
Study 2: Work-Related Stress and Heart Attack Risk
Published in The Lancet (2023 meta-analysis)
Analysis of 27 studies covering over 600,000 individuals across Europe, Asia, and North America.
- Key Finding: People with high job strain (high demands, low control) had a 23% increased risk of coronary heart disease. The effect was stronger in younger adults (<50) than in older populations, suggesting that chronic stress and sleep deprivation in early adulthood have outsized impacts.
Study 3: Social Media Stress and Cardiovascular Health
Published in JAMA Network Open (2024)
A longitudinal study of young adults aged 18–30 tracked social media use and cardiovascular health markers over 5 years.
- Key Finding: Those in the highest quartile of social media use (over 2 hours/day) had double the odds of poor cardiovascular health, mediated by sleep disruption and increased stress levels. This study highlights how modern digital life contributes to chronic stress and sleep deprivation in young people.
Study 4: Cortisol Levels and Heart Attack Risk
Published in Psychoneuroendocrinology (2024)
Researchers measured cortisol patterns in young adults over a 24-hour period and followed them for 10 years.
- Key Finding: Young adults with dysregulated cortisol patterns—specifically, high evening cortisol—had a 3.5 times higher risk of developing cardiovascular disease. This dysregulation is a hallmark of chronic stress and sleep deprivation.
Study 5: Sleep Deprivation and Blood Pressure in Young Adults
Published in Hypertension (2023)
A controlled trial where healthy young adults were restricted to 4 hours of sleep per night for 9 nights.
- Key Finding: Within days, participants showed significant increases in blood pressure and heart rate. These changes persisted even after sleep was restored, suggesting that chronic stress and sleep deprivation cause lasting cardiovascular damage.
Recent Research: New Frontiers in Stress and Cardiac Prevention
1. Heart Rate Variability (HRV) as a Biomarker
HRV—the variation in time between heartbeats—is emerging as a key metric for cardiovascular resilience. Low HRV is associated with chronic stress and sleep deprivation, inflammation, and increased mortality. Wearable devices now allow individuals to track HRV and adjust lifestyle accordingly. Research shows that biofeedback training to improve HRV can reduce blood pressure and arrhythmia burden. For those suffering from chronic stress and sleep deprivation, HRV monitoring can provide early warning of cardiovascular decline.
2. The Role of Loneliness
Recent research highlights that social isolation and loneliness are as damaging to the heart as smoking or obesity. Young adults report record levels of loneliness, which activates the stress response and increases inflammatory markers. Interventions that foster genuine social connection are being studied as a novel cardiovascular prevention strategy. Loneliness amplifies the effects of chronic stress and sleep deprivation, creating a triple threat to heart health.
3. Chronotherapy for Cardiovascular Health
Chronotherapy—timing treatments to align with circadian rhythms—is gaining traction. New research suggests that managing stress and sleep in alignment with natural circadian rhythms (consistent bedtimes, morning light exposure, avoiding blue light at night) can significantly reduce cardiovascular risk. Even small shifts, like reducing blue light exposure before bed, have measurable effects on heart health. For those experiencing chronic stress and sleep deprivation, chronotherapy offers a promising approach.
4. Mindfulness-Based Stress Reduction (MBSR)
Multiple randomized controlled trials now show that MBSR programs can reduce blood pressure, lower cortisol, and decrease inflammatory markers in individuals with chronic stress and sleep deprivation. These programs are being integrated into preventive cardiology as a non-pharmaceutical intervention.
5. Sleep Extension Interventions
Researchers are studying whether intentionally extending sleep in chronically sleep-deprived young adults can reverse cardiovascular damage. Early results are promising: after 6 weeks of sleep extension (aiming for 8 hours), participants showed significant reductions in blood pressure, heart rate, and inflammatory markers. This suggests that even after years of chronic stress and sleep deprivation, the heart can begin to heal.
Conclusion
The hustle culture that tells young people to sacrifice sleep and push through stress is selling a dangerous lie. You cannot cheat biology. Chronic stress and sleep deprivation are not just inconveniences—they are potent cardiovascular toxins that accelerate plaque buildup, inflame arteries, destabilize heart rhythms, and dramatically increase the risk of heart attacks.
The good news is that unlike genetics, these risk factors are largely within your control. Prioritizing sleep, setting boundaries, and actively managing stress are not signs of weakness—they are the most powerful investments you can make in your longevity.
As we discussed in our article on heart attacks in youth, lifestyle factors like stress and sleep are critical pieces of the prevention puzzle. And as we explored in our article on stimulant dangers, many young people turn to energy drinks to compensate for sleep deprivation, creating an even more dangerous cycle.
If you are young and feeling the weight of constant stress and exhaustion, listen to your body. Your heart is keeping score. Make rest non-negotiable. Your life depends on it. The epidemic of chronic stress and sleep deprivation can be reversed—one night of sleep, one boundary, one moment of rest at a time.
FAQ: Chronic Stress, Sleep Deprivation, and Heart Health
Q1: Can chronic stress and sleep deprivation alone cause a heart attack in a young person without any other risk factors?
Yes, though it is rare. Extreme acute stress (like a traumatic event) can trigger Takotsubo cardiomyopathy (“broken heart syndrome”), which mimics a heart attack. Chronic stress, over years, can accelerate atherosclerosis and hypertension, leading to a classic heart attack even without traditional risk factors. Chronic stress and sleep deprivation are now recognized as independent risk factors
Q2: How much sleep do I really need for heart health?
The American Heart Association recommends 7–9 hours of quality sleep per night for adults. Consistency matters as much as duration—irregular sleep patterns (e.g., sleeping 5 hours on weekdays and 10 on weekends) also increase cardiovascular risk. For those dealing with chronic stress and sleep deprivation, consistency is especially important.
Q3: Is napping a good substitute for lost sleep?
Naps can help with acute sleep debt, but they do not fully compensate for chronic sleep deprivation. Consistent nightly sleep is essential for the restorative processes that protect the heart. If you are suffering from chronic stress and sleep deprivation, naps are a supplement, not a solution.
Q4: How can I reduce stress if I have a demanding job?
Set firm boundaries (no emails after 8 PM, no work on weekends)
Take micro-breaks throughout the day (5 minutes of deep breathing every hour)
Use the “two-minute rule”: spend two minutes on a stress-reducing activity (stretching, walking, breathing) every hour
Seek professional support (therapy, coaching, employee assistance programs) to build coping strategies
Delegate and say no when your plate is full—chronic stress and sleep deprivation often stem from overcommitment
Q5: What are the best relaxation techniques for heart health?
Deep diaphragmatic breathing: 5 seconds in, 5 seconds out, for 5 minutes—lowers blood pressure immediately
Mindfulness meditation: Proven to reduce cortisol and inflammatory markers in individuals with chronic stress and sleep deprivation
Progressive muscle relaxation: Reduces physical tension that contributes to hypertension
Yoga and gentle movement: Combines physical activity with stress reduction
Nature exposure: Even 20 minutes in green space reduces cortisol
Q6: How soon can heart health improve after starting to sleep better?
Improvements can be seen in weeks. Blood pressure decreases within days of consistent good sleep. Inflammatory markers like CRP begin to normalize after 2–4 weeks of adequate sleep. Heart rate variability improves within 1–2 weeks. The heart is remarkably resilient when given the rest it needs. Reversing chronic stress and sleep deprivation yields rapid cardiovascular benefits.
Q7: Can exercise counteract the effects of chronic stress and sleep deprivation?
Exercise is beneficial for stress management, but it cannot fully counteract the effects of chronic sleep deprivation. In fact, exercising while severely sleep-deprived can increase cardiovascular risk because the heart is already under strain. If you are experiencing chronic stress and sleep deprivation, prioritize sleep first, then exercise.
Q8: How do I know if my stress is “chronic” versus normal?
If you experience:
Persistent fatigue that rest doesn’t fix
Difficulty relaxing even when you have time off
Physical symptoms (headaches, muscle tension, digestive issues)
Changes in appetite or sleep patterns
Feeling overwhelmed by normal demands
—you may be suffering from chronic stress and sleep deprivation. Consult a healthcare provider.