Introduction
The image is all too familiar: a young, seemingly invincible athlete, hydrated with a giant can of an energy drink or mixing a neon-colored pre-workout powder, ready to crush a gym session. It is a multi-billion-dollar industry built on the promise of focus, endurance, and peak performance. But behind the flashy logos and extreme-sports marketing lies a silent and growing threat to young hearts.
Emergency rooms across the country are reporting a disturbing trend: young, otherwise healthy individuals suffering sudden cardiac arrest, severe arrhythmias, and heart attacks minutes after consuming high-stimulant supplements. This is not a coincidence. The connection between these products and cardiac emergencies is becoming impossible to ignore.
While energy drinks and pre-workouts are marketed to enhance athletic performance, cardiologists are now warning that for a vulnerable subset of the population—often unaware they are vulnerable—these products can act as the final trigger for a catastrophic cardiac event. In our previous article, we explored the broader crisis of heart attacks in youth. Now, we dive deep into one of the most dangerous accelerants: stimulant supplements.
This article uncovers the five hidden mechanisms by which these popular products endanger young hearts, shares real-world cases, and provides expert guidance on how to train safely without putting your life at risk.
What Are Energy Drinks and Pre-Workout Supplements?
To understand the danger, we must first understand what these products contain. They are not simply “strong coffee.” They are complex chemical cocktails designed to push the body beyond its natural limits.
Energy Drinks
Typically sold in 16- to 24-ounce cans, energy drinks contain a combination of:
- High-dose caffeine: Often 150–300 mg per can (equivalent to 2–4 cups of coffee)
- Sugar: Up to 50–70 grams, causing rapid blood sugar spikes
- Stimulant additives: Taurine, guarana (a natural caffeine source that adds additional stimulant load), ginseng, and L-carnitine
- B-vitamins: Often in megadoses that can affect nerve function
Pre-Workout Supplements
These are powdered formulas mixed with water, taken 20–30 minutes before exercise. They often contain:
- Extreme caffeine: Some “hardcore” formulas contain 300–500 mg per scoop—enough to cause toxicity in sensitive individuals
- Beta-alanine: Causes tingling but also affects heart rate and can trigger palpitations
- Nitric oxide boosters: L-arginine and citrulline, which dilate blood vessels but can cause erratic blood pressure changes
- Yohimbine: A stimulant derived from tree bark, known to increase heart rate and blood pressure dangerously
- DMAA (1,3-dimethylamylamine): A banned stimulant still found in some products, linked to numerous cases of cardiac arrest
The problem is not just the ingredients individually, but the synergistic effect—how they interact with each other and with the physiological stress of intense exercise. This combination creates a perfect storm for cardiac arrest in young athletes.
How They Work: The Cardiovascular Cascade
To understand how a seemingly healthy athlete can collapse, we must examine what happens inside the body after consuming these products during a workout. The cascade of events can be broken down into four phases.
Phase 1: The Surge
Within 15 minutes of consumption, high-dose caffeine and other stimulants flood the bloodstream. The heart rate increases by 20–30 beats per minute or more. Blood pressure rises significantly. The body releases a surge of adrenaline, putting the cardiovascular system into a state of high alert. For individuals with undiagnosed vulnerabilities, this surge alone can trigger cardiac arrest in young athletes.
Phase 2: The Squeeze
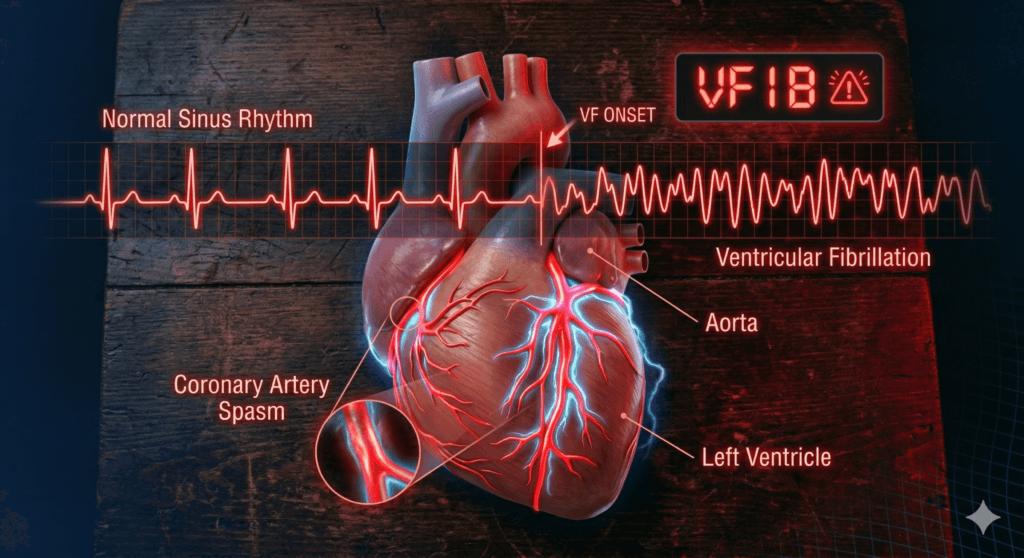
Stimulants cause vasoconstriction—the narrowing of blood vessels. While nitric oxide boosters aim to dilate vessels, the net effect in many pre-workouts is a dangerous tug-of-war. This can lead to coronary artery spasm, where the arteries supplying blood to the heart suddenly clamp down. Even without significant plaque buildup, this spasm can cause a heart attack or cardiac arrest in young athletes.
Phase 3: The Arrhythmia Trigger
Caffeine, yohimbine, and DMAA affect the heart’s electrical system. They shorten the refractory period of heart muscle cells, making them more excitable. In a person with an undiagnosed condition like Long QT Syndrome or Brugada syndrome, this can precipitate ventricular fibrillation—a chaotic heart rhythm that leads to sudden cardiac arrest. This electrical disruption is a primary mechanism behind cardiac arrest in young athletes who use these products.
Phase 4: The Dehydration Factor
Exercise causes fluid loss through sweat. Many energy drinks have a mild diuretic effect. The combination can lead to electrolyte imbalances—specifically low potassium and low magnesium. These electrolytes are essential for maintaining a normal heart rhythm. When they are depleted, the risk of arrhythmias skyrockets, setting the stage for cardiac arrest in young athletes.
Real-World Cases: When Stimulants Turn Deadly
The theoretical risks become devastatingly real when we look at documented cases of cardiac arrest in young athletes linked to energy drinks and pre-workout supplements.
Case Study 1: The College Soccer Player
Profile: Male, 19 years old. Division I soccer player. No known medical issues. Excellent physical condition.
The Event: After consuming two large energy drinks before a morning practice, he collapsed on the field during sprints. Teammates immediately began CPR. An automated external defibrillator (AED) was available on-site, and after two shocks, his heart rhythm returned to normal. He survived.
The Cause: Severe coronary artery spasm induced by massive caffeine intake combined with dehydration. Subsequent testing revealed no underlying structural heart disease—the stimulants alone triggered the cardiac arrest in young athletes. This case highlights that even those with normal hearts can be vulnerable.
Case Study 2: The “Natural” Bodybuilder
Profile: Female, 24 years old. Competitive amateur bodybuilder. Used a popular “thermogenic” pre-workout for cutting cycles. She appeared to be in peak physical condition.
The Event: She arrived at the gym, took her pre-workout, and began warming up on the treadmill. Within 10 minutes, she collapsed from sudden cardiac arrest. Despite rapid response, she did not survive.
The Cause: The supplement contained yohimbine and a high dose of caffeine. An autopsy revealed mild left ventricular hypertrophy (enlarged heart) from years of intense training, but the precipitating factor was the supplement-induced arrhythmia. This tragic case of cardiac arrest in young athletes underscores that even mild underlying conditions can become lethal when combined with stimulants.
Case Study 3: The Esports Athlete
Profile: Male, 22 years old. Professional esports athlete. Consumed energy drinks daily for focus during long gaming sessions, often consuming 3–4 cans per day.
The Event: He experienced sudden palpitations, chest tightness, and fainted at his desk during a competition. He was rushed to the hospital and diagnosed with atrial fibrillation (AFib)—an irregular, often rapid heart rate that significantly increases stroke risk.
The Cause: Chronic high consumption of energy drinks led to structural changes in the heart’s electrical pathways. AFib at 22 is almost always linked to stimulant abuse or underlying conditions. This case demonstrates that cardiac arrest in young athletes isn’t always immediate; sometimes it’s the cumulative effect of chronic use.
Case Study 4: The High School Basketball Player
Profile: Male, 17 years old. Varsity basketball player. Used a pre-workout supplement recommended by a teammate.
The Event: During a game, he collapsed after a fast break. An AED was used, and he was revived. He now has an implantable cardioverter-defibrillator (ICD).
The Cause: The supplement contained DMAA, a banned stimulant not listed on the label. DMAA is known to cause hemorrhagic stroke and cardiac arrest in young athletes. This case highlights the regulatory gaps that allow dangerous ingredients to reach consumers.
Warning Signs to Watch For
If you or someone you know uses these supplements, stop immediately and seek medical evaluation if you experience:
- Heart palpitations (feeling like the heart is skipping beats or racing)
- Chest pain or pressure during or after exercise
- Unexplained fainting or near-fainting (syncope)—this is a major warning sign for cardiac arrest in young athletes
- Severe anxiety or sense of doom after taking supplements
- Nausea or vomiting accompanying heart symptoms
- Extreme fatigue that persists despite rest
Future Impact: The Regulatory Void and a Generation at Risk
The supplement industry is largely self-regulated. Unlike prescription drugs, pre-workout supplements and energy drinks are not rigorously tested for safety by the FDA before hitting shelves. This creates a dangerous landscape where cardiac arrest in young athletes can occur from products sold legally in stores.
The “Proprietary Blend” Loophole
Manufacturers often hide the exact quantities of stimulants under the term “proprietary blend.” A consumer may think they are taking 200 mg of caffeine, but the blend could contain additional guarana and green tea extract, pushing the total stimulant load to 400 mg or more. This lack of transparency means consumers have no way of knowing their true risk of cardiac arrest in young athletes.
A Generation at Risk
As the market for “fitness optimization” grows, younger and younger consumers are being targeted. Middle school and high school athletes are now regular users of these products. Without stricter regulation and education, we will likely see a continued rise in cardiac arrest in young athletes.
The Role of Telehealth and Screening
The future of prevention lies in mandatory cardiac screening for young athletes and high-risk supplement users. Some forward-thinking sports organizations are beginning to require electrocardiograms (ECGs) for athletes, which can detect hidden electrical issues before they become catastrophic. Early identification can prevent cardiac arrest in young athletes before it happens.
Expert Opinion: Cardiologists and Toxicologists Weigh In
To understand the true risk of cardiac arrest in young athletes from stimulants, we consulted leading experts.
Dr. John Higgins, MD, Sports Cardiologist at UTHealth Houston:
“We’ve seen a dramatic increase in young patients coming in with atrial fibrillation and ventricular tachycardia directly linked to energy drink and pre-workout use. The problem is the combination—caffeine plus other stimulants plus intense exercise plus often dehydration. It’s a multiplier effect that can overwhelm even a healthy heart. This is why we’re seeing cardiac arrest in young athletes at unprecedented rates.”
Dr. Pieter Cohen, Associate Professor at Harvard Medical School, expert on supplement safety:
“Consumers have no idea what’s actually in these pre-workout powders. We’ve found synthetic stimulants like DMAA and BMPEA that were never tested for human safety. These are essentially amphetamine-like compounds hiding behind ‘natural’ marketing. They are directly linked to cardiac arrest in young athletes.”
Dr. Jennifer Ashton, MD, Chief Medical Correspondent:
“I’ve seen patients in their 20s with coronary artery spasms that were directly triggered by energy drinks. The misconception is that if it’s sold over the counter, it’s safe. That is dangerously false. We need to treat these products with the same caution we treat prescription medications, especially when considering the risk of cardiac arrest in young athletes.”
Expert Recommendations:
- Limit caffeine intake: The American Academy of Pediatrics advises that adolescents should not consume energy drinks at all.
- Read labels with skepticism: Ignore marketing buzzwords like “natural” or “clinically tested.” Look for third-party certifications like NSF Certified for Sport or Informed Choice.
- Know your baseline: Get a baseline ECG before starting intense training or using stimulant supplements, especially if you have concerns about cardiac arrest in young athletes.
- Educate young athletes: Coaches and parents must talk openly about the dangers of these products.
Recent Studies: The Data Is Alarming
The medical literature increasingly confirms the link between stimulants and cardiac arrest in young athletes.
Study 1: Energy Drinks and QT Interval
Published in Journal of the American Heart Association (2023)
Researchers studied healthy young adults who consumed 32 ounces of an energy drink within 60 minutes.
- Key Finding: The energy drink significantly prolonged the QT interval—a measure of the heart’s electrical recharge time—compared to a control drink. Prolonged QT interval is a known risk factor for life-threatening arrhythmias and cardiac arrest in young athletes.
Study 2: Pre-Workout Supplements and Emergency Department Visits
Published in Drug and Alcohol Dependence (2024)
Analyzed data from the National Electronic Injury Surveillance System.
- Key Finding: Emergency department visits related to pre-workout supplements increased by 67% over a five-year period among individuals aged 18–25. The most common complaints were chest pain, palpitations, and syncope—all warning signs for cardiac arrest in young athletes.
Study 3: The Hidden Stimulant DMAA
Published in Clinical Toxicology (2023)
Analysis of 24 pre-workout supplements sold online.
- Key Finding: 8% of products contained DMAA, a stimulant banned by the FDA for safety concerns, yet still marketed under names like “geranium extract.” DMAA has been linked to numerous cases of hemorrhagic stroke and sudden cardiac death in young adults, including cardiac arrest in young athletes.
Study 4: Cumulative Stimulant Load in Pre-Workouts
Published in JAMA Network Open (2024)
Researchers analyzed 100 popular pre-workout supplements.
- Key Finding: The average pre-workout contained the equivalent of 3–5 cups of coffee per serving, with some exceeding 500 mg of caffeine. Many also contained undisclosed stimulants. The authors concluded that these products pose a significant risk for cardiac arrest in young athletes.
Recent Research: New Approaches to Safety and Detection
1. Wearable Technology for Early Warning
Research is advancing the use of smartwatches with ECG capabilities (Apple Watch, Fitbit, Garmin) to detect arrhythmias in young athletes. Studies show that wearables can identify atrial fibrillation and other rhythm disturbances that might be triggered by stimulants, allowing for early intervention. This technology could help prevent cardiac arrest in young athletes by providing early warnings.
2. Metabolomic Profiling
New research is exploring how genetic variations affect caffeine metabolism. Individuals who are slow metabolizers (due to CYP1A2 gene variants) have a significantly higher risk of heart attack when consuming high doses of caffeine. A simple genetic test could identify who should avoid energy drinks and pre-workouts entirely, reducing the risk of cardiac arrest in young athletes.
3. The Role of Taurine Revisited
Taurine is a common additive in energy drinks, often touted as protective. However, recent animal studies suggest that high-dose taurine combined with caffeine may actually potentiate the arrhythmogenic effects, rather than reduce them. More research is needed, but the combination is now under scrutiny as a potential contributor to cardiac arrest in young athletes.
4. Regulatory Advocacy
Researchers are increasingly advocating for stricter FDA regulation of energy drinks and pre-workout supplements. Current proposals include requiring warning labels about the risk of cardiac arrest in young athletes, limiting caffeine content, and banning dangerous stimulants like DMAA and yohimbine.
Conclusion
Energy drinks and pre-workout supplements promise a shortcut to peak performance, but for a growing number of young athletes, they are a shortcut to the emergency room—or worse. The combination of massive stimulant doses, the physiological stress of exercise, and often undiagnosed genetic vulnerabilities creates a perfect storm for cardiac arrest in young athletes.
This does not mean every young person who drinks an energy drink will experience cardiac arrest. But it does mean that we must stop treating these products as harmless. They are potent drug cocktails that can unmask life-threatening conditions. As we discussed in our overview of heart attacks in youth, lifestyle factors like stimulant use are major contributors to the rising crisis.
If you are a young athlete, a parent, or a coach, the message is clear: train smart, not stimulant-fueled. Prioritize sleep, proper nutrition, and hydration. If you choose to use supplements, consult a cardiologist first—especially if you have a family history of sudden death or heart conditions. Your performance is not worth your life. The next case of cardiac arrest in young athletes could be someone you know.
FAQ: Energy Drinks, Pre-Workouts, and Heart Health
Q1: Are all energy drinks dangerous, or only when combined with exercise?
The risk is highest when combined with exercise because the heart is already under stress. However, even at rest, excessive consumption can cause high blood pressure, anxiety, and arrhythmias. For individuals with underlying heart conditions, even one energy drink at rest can trigger cardiac arrest in young athletes.
Q2: Is coffee a safer alternative?
Plain coffee in moderate amounts (1–2 cups) is generally considered safe for most people. The danger with energy drinks and pre-workouts is the combination of caffeine with other stimulants (guarana, yohimbine) and the massive doses in a short period. Coffee does not carry the same risk of cardiac arrest in young athletes.
Q3: Can I still take pre-workout if I have no symptoms?
If you have no known heart issues, it may be safe for some, but it is wise to undergo a pre-screening with a physician, including an ECG and blood pressure check. Avoid products with proprietary blends or unknown stimulants. Even without symptoms, you could be vulnerable to cardiac arrest in young athletes.
Q4: What should I do if I feel palpitations after taking a supplement?
Stop the activity immediately. Sit down, stay calm, and hydrate with water. If the palpitations persist, are accompanied by chest pain, dizziness, or fainting, call emergency services immediately. These could be warning signs of impending cardiac arrest in young athletes.
Q5: How can I boost energy for workouts naturally?
Sleep: 7–9 hours is the most powerful performance enhancer. Lack of sleep is a risk factor for cardiac arrest in young athletes.
Nutrition: A balanced meal 2–3 hours before exercise.
Hydration: Adequate water and electrolytes.
Caffeine cycling: If you use caffeine, limit it to 100–200 mg from coffee or tea, and avoid it on rest days to maintain sensitivity.
Adaptogens: Some athletes use ashwagandha or rhodiola for stress management, though consult a doctor first.
Q6: Are there any supplements that are proven safe for heart health?
For most people, creatine monohydrate (without added stimulants) is well-studied and does not negatively affect heart rhythm. Beta-alanine (again, in pure form) is generally safe. Always choose single-ingredient products from reputable third-party tested brands. Avoid anything marketed as “proprietary blend” to reduce the risk of cardiac arrest in young athletes
Q7: How common is cardiac arrest in young athletes from supplements?
While exact numbers are difficult to track due to underreporting, studies suggest that supplement use is involved in 5–10% of sudden cardiac events in young athletes. The true number may be higher because many cases go unreported. As highlighted in our article on heart attacks in youth, stimulants are a major contributor to the overall crisis.

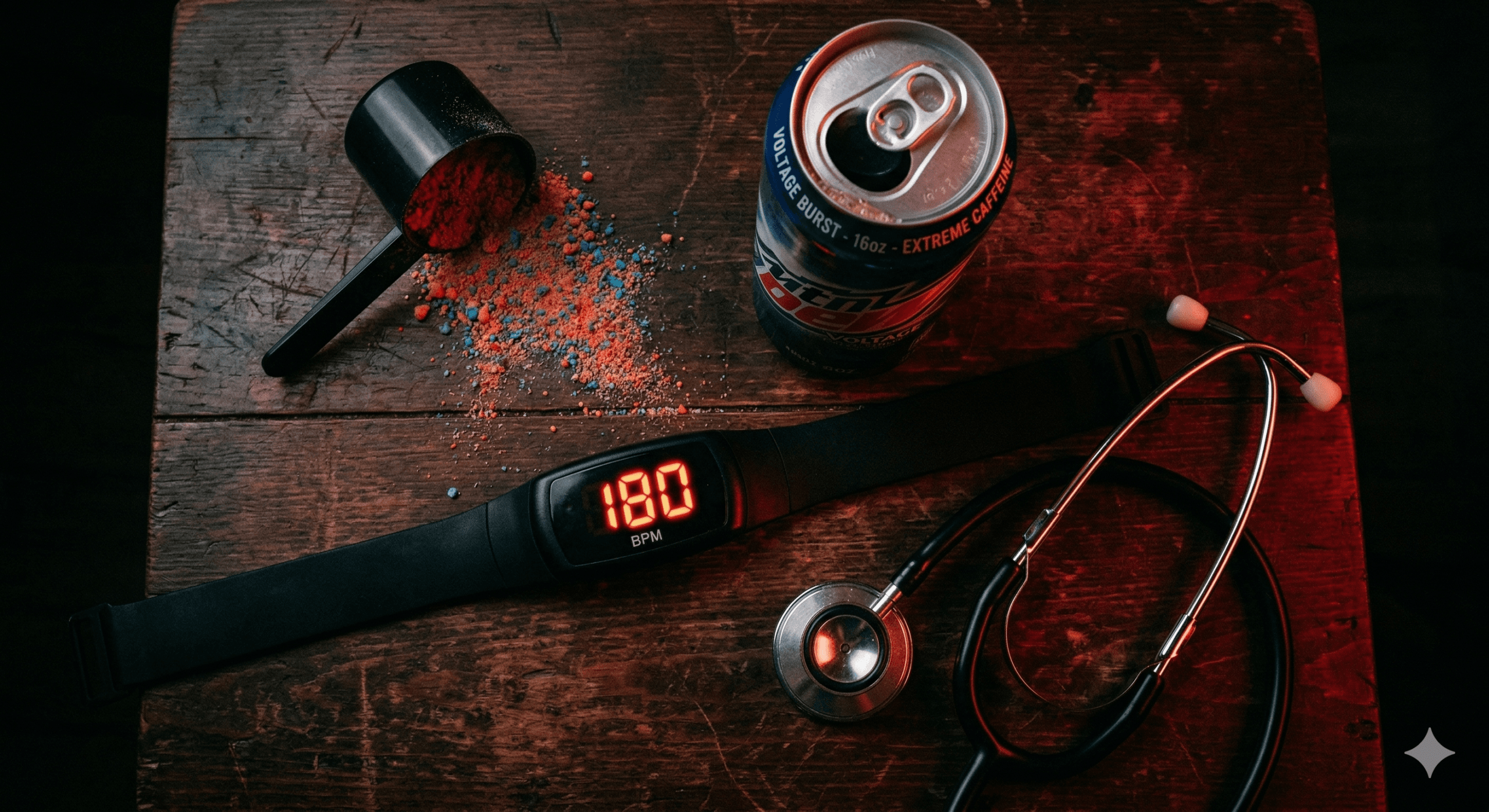




3 thoughts on “5 Hidden Ways Energy Drinks and Pre-Workout Supplements Trigger Cardiac Arrest in Young Athletes”