Introduction
For decades, heart attacks were considered a problem of old age—gray-haired individuals with a lifetime of smoking and poor diet behind them. That image is dangerously outdated.
Today, a silent epidemic is sweeping through college campuses, corporate offices, and even high school gymnasiums. Young, seemingly healthy individuals in their 20s, 30s, and early 40s are suddenly collapsing from cardiac events. The statistics are staggering: heart attacks in youth have risen by nearly 2% annually over the past decade, according to recent data. This demographic, once considered “low risk,” now accounts for a growing share of cardiovascular emergencies.
This isn’t a medical anomaly; it is a public health crisis fueled by modern lifestyles, hidden genetic vulnerabilities, and a widespread lack of awareness. If you are under 40—or you love someone who is—this is the most important article you will read this year.
We will explore the seven alarming reasons behind the surge in heart attacks in youth, decode how a heart attack actually happens, share real-world cases, and provide expert insights to help you protect yourself and your family.
What Is a Heart Attack (Myocardial Infarction) in Young Adults?
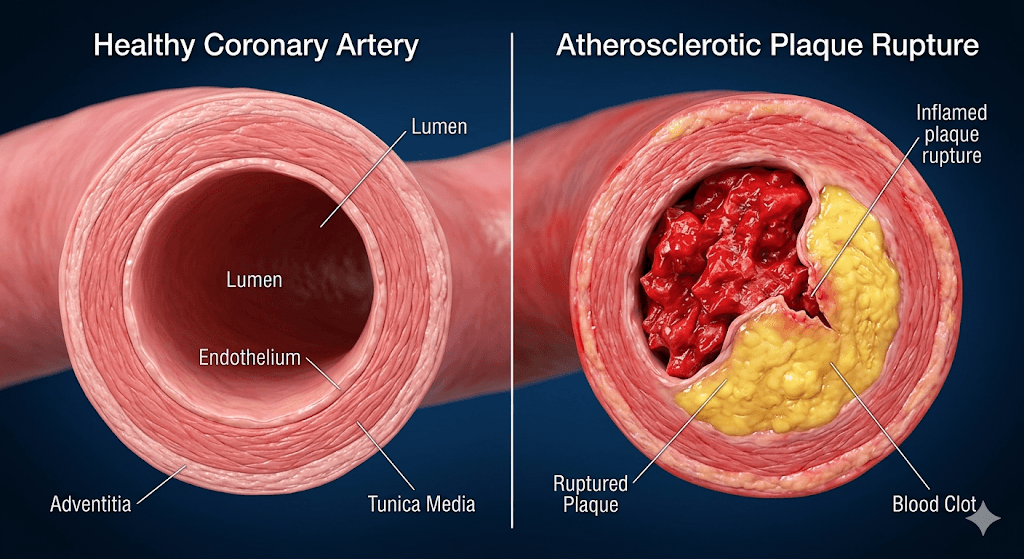
To understand why heart attacks in youth are increasing, we must first understand what a heart attack is. Contrary to popular belief, a heart attack is not the same as cardiac arrest. Instead, it is a plumbing problem.
A heart attack, medically known as a myocardial infarction, occurs when the flow of oxygen-rich blood to a section of the heart muscle is suddenly blocked. If the blockage isn’t treated quickly, the heart muscle begins to die and is replaced by scar tissue. This permanent damage can lead to debilitating heart failure or sudden death.
The “Young Heart” Myth
A pervasive myth suggests that young arteries are too elastic to clog. Unfortunately, atherosclerosis—the buildup of plaque—begins in childhood. By the time a person reaches their 20s, fatty streaks can already be forming in their arteries. For a growing number of individuals, this plaque buildup accelerates at an unprecedented rate due to modern environmental and lifestyle factors. This is why heart attacks in youth are no longer rare.
Why Heart Attacks in Youth Are Often Missed
One reason heart attacks in youth are so deadly is misdiagnosis. A 20-year-old complaining of chest pain is frequently told they are having an anxiety attack or acid reflux. This delay in treatment can be fatal. Recognizing that heart attacks in youth can present differently is crucial for survival.
How It Works: The Mechanics of a Cardiac Crisis
To visualize how heart attacks in youth occur, imagine your coronary arteries as narrow pipes. In a healthy young adult, these pipes are smooth and wide open. However, in a high-risk young adult, two primary mechanisms cause the crisis.
A. The Slow Burn: Plaque Rupture
This is the most common mechanism behind heart attacks in youth. Over years of poor diet, stress, and smoking, plaque—a waxy substance made of cholesterol, calcium, and inflammatory cells—builds up inside the artery walls.
- The Scenario: A seemingly stable plaque suddenly ruptures.
- The Reaction: The body perceives this rupture as an injury and sends platelets to “heal” the area.
- The Result: A blood clot forms rapidly, completely occluding the artery. The heart muscle below the clot is starved of oxygen. This sequence is responsible for many heart attacks in youth.
B. The Sudden Shock: Coronary Artery Spasm
This mechanism is less common but occurs more frequently in young adults with few traditional risk factors. It is a hidden cause of heart attacks in youth.
- The Scenario: Extreme stress, stimulant use (caffeine pills, energy drinks, cocaine), or severe dehydration causes the artery walls to constrict violently.
- The Result: The artery squeezes shut temporarily. Even without significant plaque buildup, the heart is starved of blood. This is often what happens to athletes who collapse on the field.
The Inflammatory Link
Modern cardiology emphasizes that inflammation is the true enemy. Cholesterol isn’t inherently dangerous unless it becomes inflamed. In youth, chronic inflammation from stress, lack of sleep, and processed foods creates an environment where the arteries are primed for disaster. This inflammatory state is a key driver of heart attacks in youth.
Real-World Uses: Case Studies and Warning Signs
Let’s move from theory to reality. These anonymized real-world examples illustrate the diverse ways heart attacks in youth manifest.
Case Study 1: The Marathon Runner
Profile: Male, 34 years old. Vegetarian, runs 10 miles a day. No family history of heart disease.
The Event: During a competitive race, he collapsed 200 meters from the finish line.
The Cause: He had a condition called Spontaneous Coronary Artery Dissection (SCAD) . A tear spontaneously formed in the wall of his coronary artery, causing a blockage. SCAD is a leading cause of heart attacks in youth, particularly in young, healthy women and men, often triggered by extreme physical exertion and hormonal fluctuations.
Case Study 2: The Corporate Grind
Profile: Female, 28 years old. Works in finance. Non-smoker, normal BMI.
The Event: After a week of 18-hour workdays fueled by energy drinks and takeout, she woke up with severe jaw pain and nausea. She thought it was the flu.
The Cause: “Burnout cardiomyopathy” (Takotsubo syndrome), often called broken heart syndrome, combined with severe electrolyte imbalance from energy drinks. The stress hormones literally “stunned” her heart muscle, resulting in one of the many heart attacks in youth linked to extreme stress.

Case Study 3: The Social Media Influencer
Profile: Male, 22 years old. Looks physically fit, uses vaping products and pre-workout supplements.
The Event: Experienced sudden palpitations and chest tightness at the gym.
The Cause: Severe LAD (Left Anterior Descending) artery blockage—the “widowmaker.” Despite his lean appearance, his lipid panel showed extremely high LDL cholesterol due to a genetic predisposition compounded by the vasoconstricting effects of nicotine and stimulants. This case underscores that heart attacks in youth can strike even those who appear fit.
Key Warning Signs You Must Know
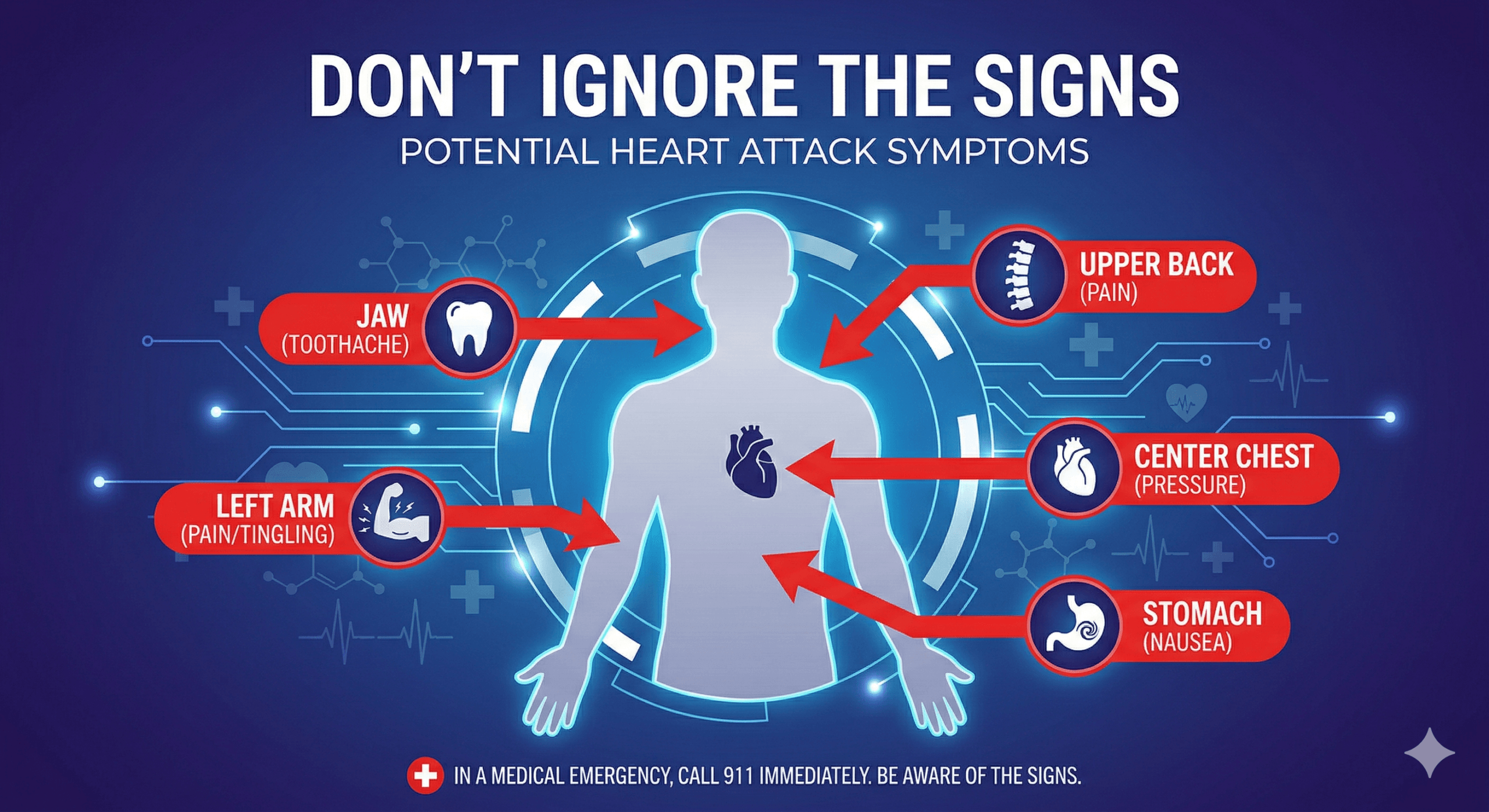
Unlike the Hollywood depiction of a man clutching his chest and falling over, symptoms of heart attacks in youth often differ, especially in women.
- Chest Discomfort: Not always pain. Often a feeling of pressure, squeezing, fullness, or burning.
- Jaw or Toothache: Unexplained pain in the lower jaw or neck, especially on the left side.
- Arm Pain: Radiating pain down the left arm, but sometimes the right arm or both.
- Stomach Pain: Nausea, vomiting, or indigestion that feels like heartburn but isn’t relieved by antacids.
- Extreme Fatigue: Unusual, sudden exhaustion despite getting adequate sleep.
- Shortness of Breath: Difficulty breathing without exertion, or during light activity.
Recognizing these atypical signs is critical because heart attacks in youth often present differently than in older adults.
Future Impact: The Burden of Early Cardiac Events
If the current trajectory continues, the future of public health looks grim. We are facing a generation that will live with chronic heart failure for 40 or 50 years rather than dying suddenly in old age. The rising incidence of heart attacks in youth will have profound consequences.
The Economic Burden
Surviving a heart attack at 30 doesn’t mean returning to a normal life. It often results in:
- Lifelong Medication: Blood thinners, beta-blockers, and statins become daily necessities.
- Reduced Earning Potential: Physical limitations may prevent a return to high-stress or physically demanding jobs.
- Mental Health Crisis: Post-traumatic stress disorder (PTSD) is extremely common after a cardiac event in young people, leading to anxiety and depression.
The “Long COVID” Connection
Emerging research suggests that viral infections, particularly COVID-19, have long-term vascular implications. Studies indicate that even mild COVID-19 infections can increase the risk of cardiovascular events—including heart attacks in youth—for up to a year post-infection. This is creating a new wave of cardiac risk in a population already vulnerable to lifestyle-induced inflammation.
Expert Opinion: Insights from Leading Cardiologists
To add depth to our analysis of heart attacks in youth, we consulted insights from leading voices in preventive cardiology.
Dr. Martha Gulati, MD, Editor-in-Chief of CardioSmart:
“We are seeing a paradigm shift. Young people today have higher rates of diabetes and obesity than their parents did at the same age. But beyond that, we are dealing with ‘psychosocial stressors’ —social media pressure, financial instability, and isolation—which release cortisol and adrenaline that literally wear down the cardiovascular system over time. This is a major contributor to heart attacks in youth.”
Dr. Sanjay Gupta, Neurosurgeon and Medical Correspondent:
(In the context of cardiac health) “The biggest risk factor for young people is underestimating their risk. I’ve seen patients who are ‘skinny fat’—they look fit in clothes, but they have visceral fat around their organs and terrible cholesterol profiles. You cannot judge heart health by looking in the mirror. That’s why heart attacks in youth often catch people off guard.”
Expert Takeaways for Prevention:
- Know Your Numbers: Don’t just know your weight. Know your LDL cholesterol, triglycerides, blood pressure, and fasting glucose.
- Exercise with Intention: High-intensity interval training (HIIT) is excellent, but recovery is crucial. Overtraining without sleep is a risk factor for arrhythmias.
- Supplements are Drugs: Cardiologists warn that “natural” pre-workout supplements and high-dose caffeine are among the leading triggers for coronary spasms in young men, contributing to heart attacks in youth.
Recent Studies: The Data You Need to See
The medical literature is catching up to the clinical reality of heart attacks in youth. Here are three pivotal recent studies.
Study 1: The ARIC Study (Atherosclerosis Risk in Communities)
Published in Circulation (2023)
This long-term study found that adults aged 35-44 saw a significant increase in heart attacks in youth rates over the past decade, reversing a previous trend of decline.
- Key Finding: Young adults who had a heart attack were significantly more likely to use marijuana and cocaine compared to older cohorts, highlighting the role of substance use in acute cardiac events.
Study 2: The Impact of Vaping
Published in Journal of the American College of Cardiology (JACC) (2024)
Researchers found that young adults who use e-cigarettes are 55% more likely to suffer a heart attack, stroke, or develop coronary artery disease compared to non-users.
- Key Finding: The chemicals in vape aerosols (not just nicotine) cause endothelial dysfunction—the inner lining of the blood vessels becomes inflamed and unable to dilate properly, increasing vulnerability to heart attacks in youth.
Study 3: Sleep and Circadian Rhythm Disruption
Published in Scientific Reports (2024)
Analyzing data from young adults with irregular sleep patterns (shift workers and “night owls”).
- Key Finding: Young adults sleeping less than 6 hours a night had a 200-300% higher risk of developing calcified plaque in their arteries compared to those sleeping 7-8 hours, independent of diet and exercise. This sleep deficit is a hidden contributor to heart attacks in youth.
Recent Research: The New Frontier in Treatment
While prevention is ideal, research into treatment for young survivors of heart attacks in youth is advancing rapidly.
1. Polygenic Risk Scores (PRS)
Traditional screening looks at family history (did your dad have a heart attack?). New research utilizes Polygenic Risk Scores. By analyzing DNA, doctors can now tell a 20-year-old if they have a high genetic predisposition to heart disease, even if their family history seems clean. This allows for early, aggressive statin therapy in the 20s, which is becoming a new standard of care for high-risk genotypes and may prevent heart attacks in youth later.
2. Colchicine for Inflammation
Colchicine, a centuries-old gout medication, has emerged as a breakthrough in cardiac care. Recent trials show that low-dose colchicine significantly reduces the risk of recurrent heart attacks by targeting the inflammatory component of plaque. For young survivors, this offers a new way to prevent a second event without the heavy side effects of traditional blood thinners.
3. Advanced Imaging (CCTA)
Standard stress tests (treadmill tests) are often inaccurate for young people, frequently producing false positives or false negatives. Recent research advocates for the use of Coronary Computed Tomography Angiography (CCTA) in young patients with suspicious symptoms. CCTA allows doctors to see the actual plaque in the artery walls, providing a definitive diagnosis that stress tests often miss. This is particularly valuable in diagnosing heart attacks in youth where traditional tests may be inconclusive.
Conclusion
The rise of heart attacks in youth is not a trend; it is a wake-up call. It dismantles the comforting myth that cardiovascular disease is a problem for “old people.” The modern world—with its ultra-processed foods, 24/7 stress culture, normalization of stimulant use, and sedentary digital lifestyles—has created the perfect storm for young arteries.
However, knowledge is power. By understanding the mechanisms of plaque rupture, recognizing atypical symptoms (like jaw pain or extreme fatigue), and aggressively managing risk factors regardless of age, we can reverse the trend of heart attacks in youth.
If you are young and feel something is “off” with your heart—if you get winded walking up stairs that used to be easy, or if you feel a fluttering in your chest—trust your instincts. Demand testing. Your age is not a shield against heart attacks in youth. Your awareness is.
FAQ: Heart Attacks in Youth
Q1: Can a healthy 25-year-old have a heart attack?
Yes. While rare, it is possible due to undiagnosed genetic conditions like hypertrophic cardiomyopathy (HCM), SCAD, or severe coronary spasms triggered by stress or stimulants. “Healthy” is not a diagnosis; it requires verification through actual biometric data. Heart attacks in youth can occur in the absence of traditional risk factors.
Q2: Are energy drinks really that dangerous?
Yes, particularly when consumed in large quantities or combined with alcohol or exercise. Energy drinks cause a “triple threat”: they increase heart rate (tachycardia), raise blood pressure, and cause platelet aggregation (stickiness of the blood), increasing the risk of clots. This mechanism can trigger heart attacks in youth.
Q3: What is the difference between a cardiac arrest and a heart attack?
This is a critical distinction. A heart attack is a circulation problem (blocked artery). A cardiac arrest is an electrical problem (arrhythmia) where the heart stops beating. A heart attack can lead to cardiac arrest. However, in many young athletes, cardiac arrest occurs without a prior heart attack due to undiagnosed structural heart defects. Understanding this distinction is important when discussing heart attacks in youth.
Q4: Can anxiety mimic a heart attack?
Absolutely. Panic attacks can cause chest pain, racing heart, sweating, and shortness of breath. However, the danger lies in dismissing a real heart attack as “just anxiety.” If symptoms are new, severe, or accompanied by cold sweats and a feeling of “impending doom,” seek emergency care immediately. Heart attacks in youth are frequently misattributed to anxiety.
Q5: What should I do if I see a young person collapse?
Call emergency services immediately. If they are unresponsive and not breathing normally, begin hands-only CPR (hard and fast in the center of the chest) and locate an Automated External Defibrillator (AED) . Time to defibrillation is the single most important factor for survival in cardiac arrest. Prompt action can save a life when heart attacks in youth lead to cardiac arrest.
Q6: How can I reduce my risk starting today?
Stop all nicotine: Vaping is just as dangerous as smoking for vascular health.
Get a baseline lipid panel: You need to know your LDL and Lp(a) levels (a genetic cholesterol factor).
Prioritize sleep: Aim for 7 hours minimum. Sleep is when the body repairs vascular tissue.
Manage stress: Chronic stress raises cortisol, which increases plaque inflammation.
Know the symptoms: Familiarize yourself with atypical signs so you can act fast if heart attacks in youth occur around you.


1 thought on “7 Alarming Reasons Why Heart Attacks in Youth Are Skyrocketing (And How to Spot the Warning Signs)”